The condition now referred to as premenstrual syndrome (PMS) has a long and varied history among medical investigators. This history dates back to the time of Hippocrates, and the first reference in a scientific journal was by Franc in 1931. In 1964, Dr. Katherina Dalton brought attention to this condition with her first book on PMS, which promoted the theory that this condition was caused by either a progesterone deficiency or an imbalance in the estrogen-progesterone ratio. Later, she also extensively promoted the use of progesterone therapy for its treatment.
While its medical and pathophysiologic components have been difficult to crystallize, PMS has been locked in with various political and legal perspectives. For example, murder convictions and felony charges have been reduced to manslaughter and misdemeanors, respectively, because of the argument that the accused woman suffered from PMS. Feminists have voiced concern about this trend indicating that the use of PMS as a defense in criminal or civil matters could result in a negative impact on women’s push toward equalization with men. Feminists plead that generalizations about women should not be made when assessing the legal or political aspects of this condition. Another point of view suggests that this condition has held back many women over the years. This should prompt interest and concern about finding the underlying causes and treating them effectively, so that those women who suffer from premenstrual syndrome are also given full access to opportunities. Furthermore, PMS is a condition that has destroyed relationships, led to divorce and child abuse and has created numerous aberrant stereotypes about the behavior of women.
The diagnosis of PMS at the Pope Paul VI Institute includes the following list of symptoms: irritability, breast tenderness, bloating, weight gain, carbohydrate craving, crying easily, depression, headaches, fatigue and insomnia. The important aspect of diagnosis is that these symptoms must begin at least four days prior to the onset of menses. If they occur within three days of the onset of menses, they are considered to be normal premenstrual molimina. In addition to these 10 core symptoms, other symptoms have also been documented in this group of patients.
By charting one’s cycle, a physician can target the postovulatory phase of the cycle with an adequate hormonal evaluation. In women who have premenstrual syndrome, both progesterone and estrogen levels, along with beta-endorphin levels, are decreased late in the cycle. These hormonal changes, as identified through research at the Pope Paul VI Institute, are shown in Figures 29-11, 29-12, and 29-13.
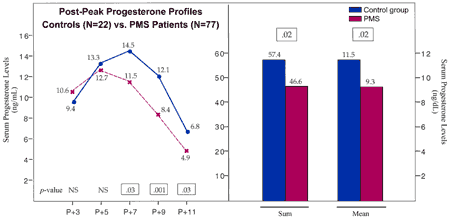
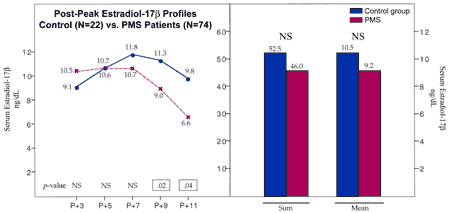
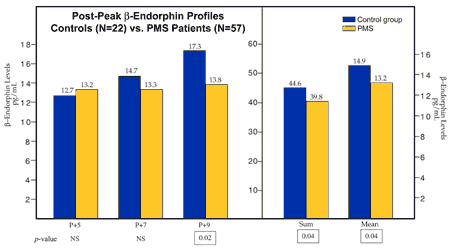
By treating these hormonal abnormalities cooperatively with either cooperative progesterone replacement therapy or targeted HCG support (which should also improve both progesterone and estrogen production) and/or with the use of naltrexone as an opiate receptor antagonist, a high degree of success can be obtained with hormonal treatment.
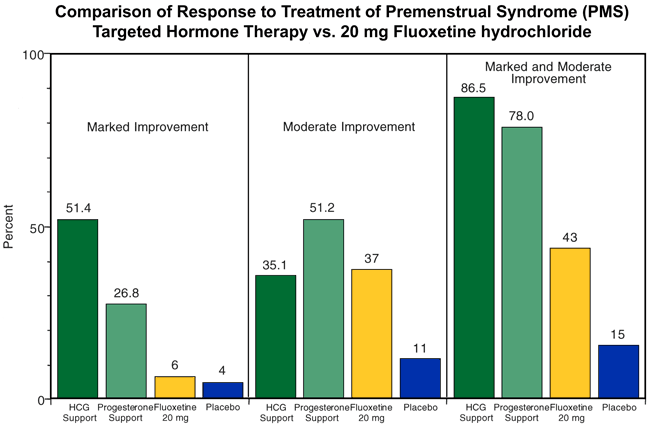
At the present time, fluoxetine (Prozac) is considered the treatment of choice for women with premenstrual syndrome. However, in comparing targeted hormonal supplementation (cooperative progesterone replacement therapy) with Prozac, the targeted hormonal therapy is significantly more effective (Figure 29-16). In addition, the treatment effect is much more rapid in onset and helps attain the normal physiology of a woman so she actually feels more normal and does not feel “drugged.”